Connect With Us
Blog
 Stress fractures in the foot are tiny cracks in the bone that happen when your feet are overworked. Unlike regular fractures that occur from a single, severe impact, stress fractures result from repetitive force over time, like running long distances or jumping repeatedly. Athletes and people who dramatically increase physical activity without proper training are more likely to develop stress fractures. After muscles are pushed to a certain point, they become fatigued and place extra stress to the bones, leading to these small cracks. Poor footwear, uneven surfaces, and weak bones from conditions like osteoporosis can increase the risk of developing stress fractures. Pain with stress fractures in the foot often worsens over time and may be experienced as a dull achy feeling. If you have sustained a stress fracture in the foot, it is suggested you make an appointment with a podiatrist promptly for treatment.
Stress fractures in the foot are tiny cracks in the bone that happen when your feet are overworked. Unlike regular fractures that occur from a single, severe impact, stress fractures result from repetitive force over time, like running long distances or jumping repeatedly. Athletes and people who dramatically increase physical activity without proper training are more likely to develop stress fractures. After muscles are pushed to a certain point, they become fatigued and place extra stress to the bones, leading to these small cracks. Poor footwear, uneven surfaces, and weak bones from conditions like osteoporosis can increase the risk of developing stress fractures. Pain with stress fractures in the foot often worsens over time and may be experienced as a dull achy feeling. If you have sustained a stress fracture in the foot, it is suggested you make an appointment with a podiatrist promptly for treatment.
Activities where too much pressure is put on the feet can cause stress fractures. To learn more, contact one of our podiatrists from Community Foot Specialists. Our doctors can provide the care you need to keep your pain free and on your feet.
Dealing with Stress Fractures of the Foot and Ankle
Stress fractures occur in the foot and ankle when muscles in these areas weaken from too much or too little use. The feet and ankles then lose support when walking or running from the impact of the ground. Since there is no protection, the bones receive the full impact of each step. Stress on the feet can cause cracks to form in the bones, thus creating stress fractures.
What Are Stress Fractures?
Stress fractures occur frequently in individuals whose daily activities cause great impact on the feet and ankles. Stress factors are most common among:
- Runners
- People affected with Osteoporosis
- Tennis or basketball players
- Gymnasts
- High impact workouts
Symptoms
Pain from the fractures occur in the area of the fractures and can be constant or intermittent. It will often cause sharp or dull pain with swelling and tenderness. Engaging in any kind of activity which involves high impact will aggravate pain.
If you have any questions please feel free to contact our offices located in Beavercreek, Dayton, and Vandalia, OH . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Our bones are important aspects of our body and they are constantly changing. The heavier the workload for a bone, the more likely it is that calcium will be placed in it. When a bone isn’t used often, there won’t be much calcium within it. When stress from repetitive loads prevent the bone from being able to repair itself, cracks will start to form. Stress fractures are defined as cracks in a bone that result from repetitive force, such as overuse.
The most common cause of stress fractures is a sudden increase in intensity and duration of physical activity. For example, if you begin to run long distances without working your way into doing so, you will be more likely to develop a stress fracture.
Common symptoms of stress fractures are pain and swelling near the weight bearing area on the injured bone. When initial x-rays are performed, it is possible that the fracture will not show up. However, once the stress on the area continues, the damage will increase, and the fracture will be severe enough to show up on an x-ray. Certain parts of the foot are more likely to develop stress fractures than others. Areas that typically have these fractures are: the metatarsals, the navicular bone, the calcaneus, tibia, and fibula.
Since women are at an increased risk of developing osteoporosis, they are twice as likely as men to sustain a stress fracture. Additionally, old age causes a decrease in bone mineral density which is why elderly people are also likely to develop these fractures.
It is important for you to be professionally diagnosed by a podiatrist if you suspect you have a stress fracture, because there are other injuries that can easily be mistaken for a fracture. Sprains, strains, shin splints, plantar fasciitis, and Morton’s neuroma can all easily be mistaken for stress fractures in the foot. Your podiatrist will likely ask you a series of questions to determine what type of pain you are experiencing. These questions will help your doctor identify whether you have a stress fracture.
The best method of treatment for a stress fracture is rest. Additionally, a walking boot, cast, or crutches, will help rest the area that is injured. The typical healing time for stress fractures is 4-12 weeks, however this depends on which bone is involved.
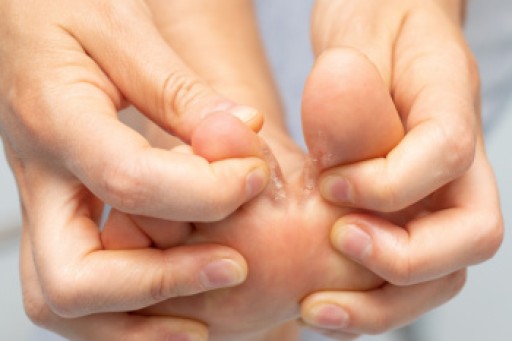
 Athlete's foot, a fungal skin infection of the foot, can become severe and cause blisters or ulcers. Severe athlete’s foot can be a persistent and debilitating condition that significantly impacts a patient’s quality of life. The advanced stage of the infection is characterized by intense itching, burning, and a noticeable degradation of the skin on the feet. This includes cracking, peeling, and the emergence of blisters. Ulcers, or deep sores, may appear on the heel or ball of the foot. Where athlete’s foot normally appears between the toes or the side of the foot, severe athlete's foot may spread beyond these areas to the rest of the foot. This can lead to secondary bacterial infections due to the compromised integrity of the skin. Treatment usually includes a multi-step approach, such as prescribed antifungal medications, rigorous hygiene practices, and possibly lifestyle adjustments. If you suspect athlete’s foot, it is suggested that you make an appointment with a podiatrist promptly to prevent the condition from worsening.
Athlete's foot, a fungal skin infection of the foot, can become severe and cause blisters or ulcers. Severe athlete’s foot can be a persistent and debilitating condition that significantly impacts a patient’s quality of life. The advanced stage of the infection is characterized by intense itching, burning, and a noticeable degradation of the skin on the feet. This includes cracking, peeling, and the emergence of blisters. Ulcers, or deep sores, may appear on the heel or ball of the foot. Where athlete’s foot normally appears between the toes or the side of the foot, severe athlete's foot may spread beyond these areas to the rest of the foot. This can lead to secondary bacterial infections due to the compromised integrity of the skin. Treatment usually includes a multi-step approach, such as prescribed antifungal medications, rigorous hygiene practices, and possibly lifestyle adjustments. If you suspect athlete’s foot, it is suggested that you make an appointment with a podiatrist promptly to prevent the condition from worsening.
Athlete’s Foot
Athlete’s foot is often an uncomfortable condition to experience. Thankfully, podiatrists specialize in treating athlete’s foot and offer the best treatment options. If you have any questions about athlete’s foot, consult with one of our podiatrists from Community Foot Specialists. Our doctors will assess your condition and provide you with quality treatment.
What Is Athlete’s Foot?
Tinea pedis, more commonly known as athlete’s foot, is a non-serious and common fungal infection of the foot. Athlete’s foot is contagious and can be contracted by touching someone who has it or infected surfaces. The most common places contaminated by it are public showers, locker rooms, and swimming pools. Once contracted, it grows on feet that are left inside moist, dark, and warm shoes and socks.
Prevention
The most effective ways to prevent athlete’s foot include:
- Thoroughly washing and drying feet
- Avoid going barefoot in locker rooms and public showers
- Using shower shoes in public showers
- Wearing socks that allow the feet to breathe
- Changing socks and shoes frequently if you sweat a lot
Symptoms
Athlete’s foot initially occurs as a rash between the toes. However, if left undiagnosed, it can spread to the sides and bottom of the feet, toenails, and if touched by hand, the hands themselves. Symptoms include:
- Redness
- Burning
- Itching
- Scaly and peeling skin
Diagnosis and Treatment
Diagnosis is quick and easy. Skin samples will be taken and either viewed under a microscope or sent to a lab for testing. Sometimes, a podiatrist can diagnose it based on simply looking at it. Once confirmed, treatment options include oral and topical antifungal medications.
If you have any questions, please feel free to contact our offices located in Beavercreek, Dayton, and Vandalia, OH . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Athlete’s foot is a type of fungal infection that affects the skin on the feet. It is caused when the tinea fungus grows on the foot. It is possible to catch the fungus through direct contact with someone who has it or by touching a surface that is contaminated with it. This type of fungus thrives in warm, moist environments such as showers, locker room floors, and swimming pools. Your risk of getting it may also increase by wearing tight-fitting, closed-toe shoes, or by having sweaty feet.
Symptoms of athlete’s foot include itching, stinging or burning sensations between the toes. You may also experience toenails that are discolored, thick, crumbly, or toenails that pull away from the nail bed.
Your podiatrist may diagnose athlete’s foot by detecting these symptoms or by doing a skin test to see if there is a fungal infection present. The most common exam used to detect Athlete’s foot is a skin lesion potassium hydroxide exam. To use this method, your doctor will scrape off a small area of the infected skin and place it into potassium hydroxide. The potassium hydroxide will destroy the normal cells and leave the fungal cells untouched so that they are visible under a microscope.
There are a variety of treatment options for athlete’s foot. Some medications are miconazole (Desenex), terbinafine (Lamisil AT), clotrimazole (Lotrimin AF), butenafine (Lotrimin Ultra), and tolnaftate (Tinactin). While these options may be able to treat your fungus, it is best that you consult with a podiatrist in order to see which treatment option may work best for you.
In some cases, Athlete’s foot may lead to complications. A severe complication would be a secondary bacterial infection which may cause your foot to become swollen, painful, and hot.
There are ways that you can prevent athlete’s foot. Washing your feet with soap and water each day and drying them thoroughly is an effective way to prevent infections. You also shouldn’t share socks, shoes, or towels with other people. It is crucial that you wear shower sandals in public showers, around swimming pools, and in other public places. Additionally, you should make sure you wear shoes that can breathe and change your socks when your feet become sweaty. If you suspect that you have Athlete’s foot, you should seek help from a podiatrist as soon as possible.

Caring for your feet becomes more important as you age, as feet impact your ability to stay upright and mobile. Research indicates that foot pain, and common issues such as bunions, are significant contributors to falls among older adults. Studies also reveal that foot pain correlates with indoor falls, affecting gait and balance. Addressing foot problems through exercises, proper footwear, and wearing orthotics can reduce fall risks. Simple exercises, like toe rotations and ankle stretches, can strengthen muscles and improve flexibility. Custom-made orthotics and choosing well-fitting shoes, especially for wider or misaligned feet, can help with comfort and balance. If you are a senior and want to prevent falling from injuring your feet, it is suggested that you schedule appointments with a podiatrist. This type of doctor can give you regular examinations and more information on foot care that can enhance mobility, independence, and overall well-being as you age.
Preventing falls among the elderly is very important. If you are older and have fallen or fear that you are prone to falling, consult with one of our podiatrists from Community Foot Specialists. Our doctors will assess your condition and provide you with quality advice and care.
Every 11 seconds, an elderly American is being treated in an emergency room for a fall related injury. Falls are the leading cause of head and hip injuries for those 65 and older. Due to decreases in strength, balance, senses, and lack of awareness, elderly persons are very susceptible to falling. Thankfully, there are a number of things older persons can do to prevent falls.
How to Prevent Falls
Some effective methods that older persons can do to prevent falls include:
- Enrolling in strength and balance exercise program to increase balance and strength
- Periodically having your sight and hearing checked
- Discuss any medications you have with a doctor to see if it increases the risk of falling
- Clearing the house of falling hazards and installing devices like grab bars and railings
- Utilizing a walker or cane
- Wearing shoes that provide good support and cushioning
- Talking to family members about falling and increasing awareness
Falling can be a traumatic and embarrassing experience for elderly persons; this can make them less willing to leave the house, and less willing to talk to someone about their fears of falling. Doing such things, however, will increase the likelihood of tripping or losing one’s balance. Knowing the causes of falling and how to prevent them is the best way to mitigate the risk of serious injury.
If you have any questions, please feel free to contact our offices located in Beavercreek, Dayton, and Vandalia, OH . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Elderly Americans are very susceptible to falls as they get older. Everyone experiences decreases in flexibility, balance, strength, and the senses as they age. This correlates to some eye-opening statistics. 1 in 4 Americans aged 65 and older fall each year. An elderly American is being treated for a fall in an emergency room every 11 seconds. In light of these striking statistics, one can see the importance of taking steps to prevent falls.
Finding an exercise program for the elderly is an excellent way to reduce the likelihood of falls. Look for an exercise program that improves strength and balance. Elderly people who live a more sedentary lifestyle, with little physical activity, are at an increased risk of falling. Wearing well-fitted footwear that provides good foot support and cushion will help prevent falls from poorly fitted shoes. Talking to a podiatrist about your susceptibility to falls and about inspecting your prescriptions will help to avoid any medication that could make falls more likely. Due to a decline in the senses among the elderly, having your eyes and hearing checked is recommended.
Around half of all falls occur in the household. Removing tripping hazards in the home and making it more accommodating to older persons can significantly reduce falls. Some notable household changes include increasing lighting around the house, installing grab bars in the shower and bathroom, and making sure the floor is clear of clutter. Other smart options include installing a shower chair, using rubber-bottomed rugs, and placing railings on both sides of stairwells.
Finally, discuss with a doctor and your family about your fear of falling. This will help to increase awareness among the population on the need for fall prevention. A lack of awareness on the matter, and a downplaying of importance are what increase the risks of falling. Following these tips can help to reduce the risk for yourself and your loved ones.
One out of ten broken bones is reported to be in the feet. When an object crushes, bends, or stretches the bone beyond acceptable ranges, bones break. A break in the foot is either a fracture or a straight break.
The location of any break can tell you how the break happened. Toes, for instance, break typically as a result of something being kicked hard and with great force. Heel breaks almost always are a result of an improper landing from a tall height. Twists or sprains are the other two frequent occurrences. As with all usual breaks, they result from unexpected accident or sudden injury. As with stress fractures, breaks form as a process over time from repeated stress on already present cracks. Runners, dancers, and gymnasts are the usual athletes who receive this type of break. Stress fractures result from incredible pressure on the feet. It is no surprise these athletes bear the majority of reported fractures.
Pain, swelling, bruising, and redness are all indicative of the typical symptoms from a broken foot. Severe pain—to the point of not being able to walk—usually depends on the location of the break in the foot. Toes are on the lower scale of pain threshold, but heels are high, as are a few other particular bones. As the severity of the broken foot increases, symptoms like blueness, numbness, misshaping of the foot, cuts, or deformities will become apparent. These symptoms indicate the need to see a medical professional with access to an x-ray facility.
Prior to seeing a specialist, precautions should be taken to reduce pain and swelling. Elevate and stabilize the foot, and refrain from moving it. Immobilization of the foot is the next priority, so creating a homemade splint is acceptable. Keep in mind that while creating a splint, any increase of pain or cutting off blood circulation means that the splint should be removed immediately. Use ice to decrease swelling and relieve pain symptoms.
When dealing with a medical center, the patient should note that the treatment can vary. The treatment will depend on the severity of the fracture and the cause of the break. Crutches, splits, or casts are common treatments while surgery has been known to be used in more severe cases in order to repair the break in the bones.
 The main symptoms of a broken foot are severe pain, swelling, and bruising around the injured area. Some patients may experience very intense pain when touching or applying pressure to the foot. Difficulty or inability to bear weight on the foot, along with visible deformities or changes in foot shape, can also indicate a potential break. Numbness of the foot is another possible symptom. X-rays or other imaging tests are commonly used to confirm the presence of a fracture. Taking immediate steps to address a potential broken foot can lead to a more effective recovery and prevent complications down the line. If you have a painful foot and suspect a break or fracture, it is suggested that you make an appointment with a podiatrist for an accurate diagnosis and appropriate treatment.
The main symptoms of a broken foot are severe pain, swelling, and bruising around the injured area. Some patients may experience very intense pain when touching or applying pressure to the foot. Difficulty or inability to bear weight on the foot, along with visible deformities or changes in foot shape, can also indicate a potential break. Numbness of the foot is another possible symptom. X-rays or other imaging tests are commonly used to confirm the presence of a fracture. Taking immediate steps to address a potential broken foot can lead to a more effective recovery and prevent complications down the line. If you have a painful foot and suspect a break or fracture, it is suggested that you make an appointment with a podiatrist for an accurate diagnosis and appropriate treatment.
A broken foot requires immediate medical attention and treatment. If you need your feet checked, contact one of our podiatrists from Community Foot Specialists. Our doctors can provide the care you need to keep you pain-free and on your feet.
Broken Foot Causes, Symptoms, and Treatment
A broken foot is caused by one of the bones in the foot typically breaking when bended, crushed, or stretched beyond its natural capabilities. Usually the location of the fracture indicates how the break occurred, whether it was through an object, fall, or any other type of injury.
Common Symptoms of Broken Feet:
- Bruising
- Pain
- Redness
- Swelling
- Blue in color
- Numbness
- Cold
- Misshapen
- Cuts
- Deformities
Those that suspect they have a broken foot shoot seek urgent medical attention where a medical professional could diagnose the severity.
Treatment for broken bones varies depending on the cause, severity and location. Some will require the use of splints, casts or crutches while others could even involve surgery to repair the broken bones. Personal care includes the use of ice and keeping the foot stabilized and elevated.
If you have any questions please feel free to contact our offices located in Beavercreek, Dayton, and Vandalia, OH . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
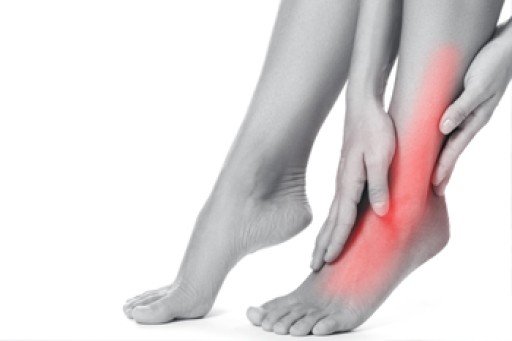
The feet, being the foundation of the body, carry all of the body’s weight and are therefore prone to experiencing pain and discomfort. If you are experiencing foot pain, it is important to determine where in the foot you are experiencing this pain to help discover the cause of it. While pain can be experienced virtually anywhere in the foot, the most common sites of foot pain are in the heel and ankle.
Heel pain can be due to a multitude of conditions including plantar fasciitis, Achilles tendinitis, and heel spurs. Pain experienced in the ankle can be a sign of an ankle sprain, arthritis, gout, ankle instability, ankle fracture, or nerve compression. In more serious cases, pain in the foot can be a sign of improper alignment or an infection.
Foot pain can be accompanied by symptoms including redness, swelling, stiffness and warmth in the affected area. Whether the pain can be described as sharp or dull depends on the foot condition behind it. It is important to visit your local podiatrist if your foot pain and its accompanying symptoms persist and do not improve over time.
Depending on the location and condition of your foot pain, your podiatrist may prescribe certain treatments. These treatments can include but are not limited to prescription or over-the-counter drugs and medications, certain therapies, cortisone injections, or surgery.
If you are experiencing persistent foot pain, it is important to consult with your foot and ankle doctor to determine the cause and location. He or she will then prescribe the best treatment for you. While milder cases of foot pain may respond well to rest and at-home treatments, more serious cases may take some time to fully recover.